By Chad Ruoff, M.D.
Let's face it: Adapting and adhering to a CPAP (continuous positive airway pressure) machine can be challenging. Take, for example, a patient we will refer to as Joe, a gentleman in his 50s who was referred to the Stanford Sleep Center by his primary care physician at the behest of his partner. In spite of wearing earplugs, his partner found his snoring intolerable. Joe, in addition to his partner's complaints, admitted to increasingly more difficulty remaining alert throughout the day. He recently started napping at work, sometimes unintentionally, and spending more time in bed at night. A common misconception, he had been attributing these difficulties to the normal process of aging.
It turned out that eights years prior, Joe had already been diagnosed with "severe" obstructive sleep apnea and prescribed a CPAP machine to treat his sleep apnea. His experiences with CPAP were not atypical, recalling quite the struggle to adapt to the device -- wearing it a couple of hours per night and only trying it a few nights per week for a month or so. Joe, not knowing any better, had not followed up with the prescribing physician to discuss his difficulty adapting to the CPAP machine. He finally gave up and returned the CPAP machine.
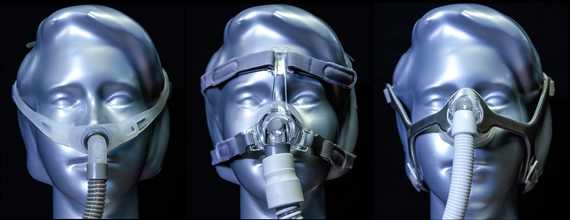
On detailed questioning he reported the full-face mask was, "just too big, leaked too much, and left marks on his face." He was never told that masks are available in different sizes and, more importantly, can come in different styles, including nasal pillows and nasal triangular devices.
He described a bloating sensation in his abdomen, sometimes associated with cramping, belching, and flatulence, whenever he wore the CPAP machine for a few hours. Referred to as aerophagia, these symptoms are frequently endorsed by CPAP users and typically respond to a decrease in the CPAP pressure. A decrease in CPAP pressure, however, may prevent the CPAP from maintaining airway patency and can lead to serious health consequences. As such, any changes in CPAP pressure require a discussion with a physician and a prescription.
A dry mouth, Joe recalled, was also one of the more uncomfortable issues hindering his use of the CPAP. Dry mouth is one of the more commonly reported side effects from CPAP. Dry mouth, often due to the mouth opening leading to air rushing out of the mouth during sleep, may improve with the use of a chinstrap, to hold the mouth closed while wearing the CPAP. A full-face mask, change in CPAP pressure, or the addition of or modification of humidification settings may also help with dry mouth.
For Joe, we decided to order a repeat overnight sleep study in our sleep center. The sleep study confirmed he had very significant sleep apnea, placing him at an increased risk of stroke and heart attack. The sleep study determined optimal CPAP settings and the best fitting mask for him. In the first week, Joe had trouble using his CPAP machine for more than one hour. However, after contacting our office, we reeducated him about the "ramp" feature of the device, which starts the CPAP at a lower pressure for patient comfort and gradually increases the pressure to the prescribed pressure over a set period of time. After these adjustments he started to use the machine more and more. He also ended up changing from a nasal triangular mask to nasal pillows.
After a month of use, he returned to see me and reported he felt more awake during the day. Review of objective data from his CPAP machine (stored on an SD data card), which is available for download from modern CPAP machines, demonstrated he was using the device for about four hours each night.
Joe's story serves as a reminder to both patients and physicians that adapting and adhering to CPAP is not easy. In fact, research shows that anywhere from 30 to 80 percent of patients have trouble adhering to at least four hours of use each night. It is important for both patients and physicians to set realistic expectations for CPAP use. Patients are encouraged to follow up with a physician with expertise in the diagnosis and treatment of sleep apnea. Had Joe followed up with a physician with expertise in sleep medicine (i.e., a board-certified sleep specialist), he might have had a different outcome eight years ago. CPAP machines and mask interfaces, as well as our understanding of alternative treatment options for sleep apnea, have improved over the last 19 years so patients who have tried CPAP in the past but failed to adapt and adhere to therapy are encouraged to discuss this with a physician, particularly a board-certified sleep specialist.
Chad Ruoff, M.D., is board-certified in internal medicine, sleep medicine, and obesity medicine and serves as a clinical assistant professor at the Stanford Center for Sleep Sciences and Medicine. This Center is the birthplace of sleep medicine and includes research, clinical, and educational programs that have advanced the field and improved patient care for decades. To learn more, visit us at: http://sleep.stanford.edu/.